Sleep apnea does far more than interrupt your nights. It disrupts cytokine production, suppresses natural killer cell activity, and sustains chronic low-grade inflammation every single night. The result is an immune system that cannot protect you properly. Research shows even a few nights of sleep deprivation cuts immune cell activity by up to 72%. Treating your sleep apnea is directly treating your immune health.
The Immune System’s Dependency on Deep Sleep
Your immune system does not run on autopilot. It requires active biological maintenance, and the window for that maintenance is sleep, specifically the deep NREM and REM stages that obstructive sleep apnea systematically destroys.
During deep sleep, the body produces and releases cytokines, the signaling proteins that coordinate immune responses, direct white blood cells to infection sites, and regulate inflammation. T-cells activate. Natural killer (NK) cells consolidate. Immunological memory from previous exposures to pathogens gets reinforced.
When sleep apnea disrupts the immune system by fragmenting these stages night after night, every one of those processes degrades. The Sleep Foundation confirms that poor sleep immune function creates a bidirectional problem: poor sleep weakens immune defenses, and a compromised immune system can make sleep quality worse. Source: Sleep Foundation
How Obstructive Sleep Apnea Disrupts Immune Function
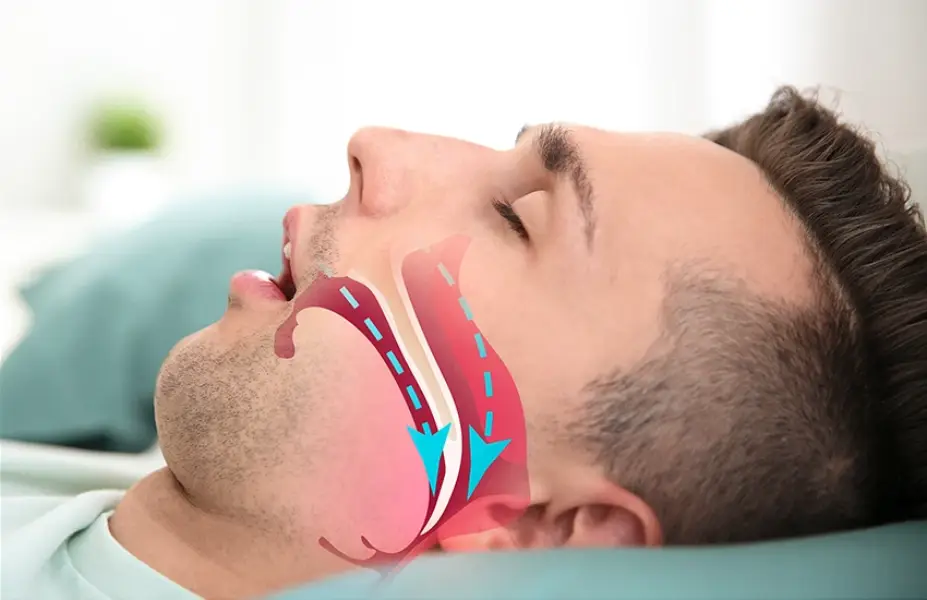
Obstructive sleep apnea is not simply a snoring problem or a nuisance condition. Every apnea event, and there can be dozens or hundreds per hour, causes a measurable drop in blood oxygen. The brain detects this, triggers a stress arousal to resume breathing, and the cycle repeats all night.
This chronic intermittent hypoxia creates a unique immunological stressor. The repeated oxygen desaturations drive oxidative stress at the cellular level, triggering inflammatory pathways that would not otherwise activate during rest.
The immunological damage from untreated OSA includes:
- Elevated C-reactive protein (CRP) and interleukin-6 (IL-6), key markers of systemic inflammation
- Reduced production of protective anti-inflammatory cytokines
- Impaired T-cell proliferation and responsiveness
- Weakened antibody response to vaccines and infections
Scientific evidence shows that even a few nights of sleep deprivation immune response suppression reduces immune cell activity by up to 72%. Nothing produces that level of sustained sleep deprivation as consistently as untreated obstructive sleep apnea inflammation. Source: Sleep Apnea KC
The Cytokine Dysregulation Problem
Cytokines are the immune system’s communication network. They tell white blood cells where to go, when to multiply, and how aggressively to respond. In a healthy, well-rested person, cytokine levels follow a regulated circadian rhythm, rising and falling in sync with sleep stages.
In patients with untreated OSA, this regulation breaks down entirely. OSA cytokine dysregulation has been confirmed across multiple NIH-published studies. A 2022 paper in PMC on cellular immune dysfunction in sleep apnea confirmed that cytokine profiles in OSA patients are consistently abnormal: pro-inflammatory cytokines are elevated while protective responses are suppressed. Source: PMC/NIH
A comprehensive 2025 review published in Frontiers in Immunology further detailed how the mechanistic pathway from OSA’s intermittent hypoxia to immune cell dysfunction is now well-established, with clinical implications across multiple chronic disease categories. Source: PMC/NIH
Sleep Apnea and NK Cell Suppression
Natural killer (NK) cells are your immune system’s first responders. They identify and destroy virus-infected cells, abnormal cells, and early-stage cancer cells before adaptive immunity even activates.
Sleep apnea NK cell suppression is one of the most consistently documented immunological effects of OSA. Chronic sleep fragmentation reduces NK cell cytotoxic activity, leaving the body exposed during the window between pathogen exposure and the activation of slower adaptive immune responses.
For people who notice they catch every cold that circulates in the office, or who seem to get sick more frequently than colleagues doing the same work in the same environment, NK cell suppression from undiagnosed OSA is a clinical possibility worth investigating.
Sleep Apnea and Autoimmune Disease
Research from the University of Georgia established that sleep apnea autoimmune disease risk is directly connected through the same cytokine dysregulation pathways. The abnormal immune signaling created by chronic OSA generates the conditions under which the immune system begins to misidentify the body’s own tissues as threats.
Conditions including rheumatoid arthritis, lupus, psoriasis, and inflammatory bowel disease have all been linked to sleep-disordered breathing in observational studies. Source: Medical News Today
A 2024 SLEEP conference study identified a genetic association between OSA and asthma, suggesting that dysregulated immune pathways from OSA create shared susceptibility across multiple chronic inflammatory conditions. Source: DocWire News
Signs Your Immune System Is Failing
The body communicates immune suppression clearly. Watch for:
- Catching colds or infections more frequently than others around you
- Illness that lingers longer than expected
- Wounds, cuts, or skin irritations that heal slowly
- Recurring oral sores or throat infections
- Persistent fatigue between illnesses
- Worsening seasonal allergies year on year
If these symptoms accompany snoring, unrefreshing sleep, or afternoon energy crashes, your immune system and your airway may share the same root cause.
The Vicious Cycle: How Illness Worsens Sleep Apnea
One of the most important aspects of sleep apnea chronic inflammation is that it sustains itself. Compromised immunity makes you more susceptible to respiratory infections. Nasal congestion, throat inflammation, and upper airway swelling from repeated infections then worsen the airway obstruction responsible for your sleep apnea.
Patients who treat their OSA consistently report breaking this cycle: fewer illnesses, faster recovery, and significantly fewer sick days per year.
Can Treating Sleep Apnea Restore Immune Health?
Yes, and the clinical evidence supports this clearly. When sleep apnea treatment restores deep sleep stages and eliminates the oxygen desaturations that drive immune dysfunction, cytokine profiles normalize, NK cell activity recovers, and systemic inflammation markers decline.
This is not a gradual or subtle effect. Patients frequently describe a marked improvement in how often they get sick and how quickly they recover once treatment begins.
LHDM Dubai: Sleep Apnea Treatment That Protects Your Health
At Leila Hariri Dental and Sleep Apnea Clinic, our dental sleep apnea treatment in Dubai uses custom oral appliance therapy as a CPAP-free approach to treating obstructive sleep apnea. By keeping your airway open throughout the night, it gives your immune system the uninterrupted deep sleep it needs to function properly.
If you are tired of being sick, slow to recover, or running on a compromised immune system, the answer may not be another supplement. It may be your airway.